Dermatology
The specialty of Dermatology and Venereology covers both the dermatological aspect, which involves the diagnosis, treatment, and follow-up of skin diseases as well as conditions related to hair and nails, and the venereological aspect, which includes the study, treatment, and research of sexually transmitted diseases.
It is a medical-surgical specialty, encompassing both clinical and surgical approaches.
- Dr. André Laureano
- Dr. Carlos Clerins
- Dra. Virginia Coelho de Sousa
- Dra. Christine Schoutens
- Dra. Christine Schoutens
- Dra. Bárbara Roque Ferreira
- Dra. Cristina da Silva Sousa
- Dr. De Lorenzo
- Dr. Vitor Neto
- Dr. Bruno Duarte
- Dr. Pedro Vale Fernandes
Hospital Particular do Algarve - Alvor
Centro Médico Internacional - VRSA
Clínica Particular de Lagos
Clínica Particular SIIPEMOR - S. Brás Alportel
Clínica Particular de Vilamoura
Instituto HPA - Montenegro – Faro
Hospital Particular do Alentejo - Sines
Madeira Medical Center
Main Dermatological Conditions:
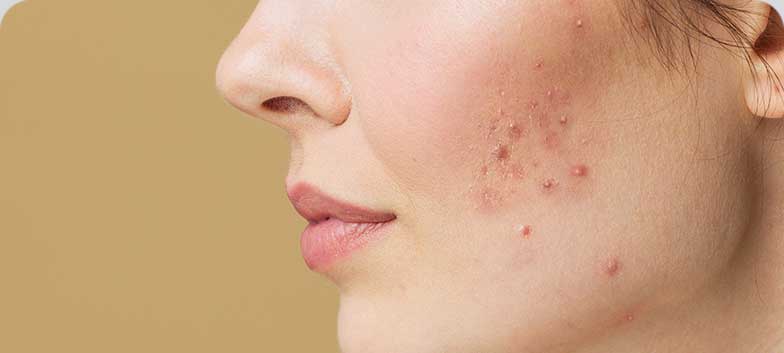
Acne
Acne is a very common skin condition that affects most adolescents, but it is not limited to them. The main changes occurring in the skin and hair are related to hormonal activity that begins during this period.
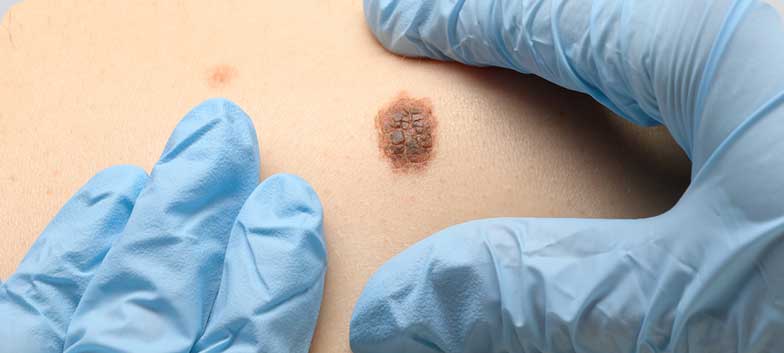
Skin Cancer
Skin cancer is caused by the abnormal and uncontrolled growth of the cells that make up the skin. These cells are arranged in layers, and depending on the affected layer, different types of cancer are defined. The most common are basal cell carcinoma and squamous cell carcinoma. Rarer and more lethal than these carcinomas is melanoma, the most aggressive type of skin cancer.

Contact Dermatitis or Eczema
Contact dermatitis is an inflammatory reaction of the skin caused by exposure to an irritant or allergen. There are two types of contact dermatitis: irritant and allergic. Although not contagious or dangerous, it can be very uncomfortable and significantly affect patients’ quality of life.
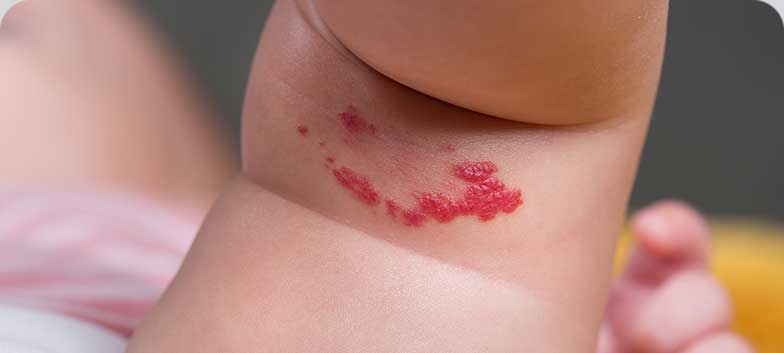
Haemangioma
Haemangiomas are benign tumoural formations of capillaries and blood vessels. They appear on the skin as red or purplish spots or lumps. While they may represent only cosmetic concerns, those present from birth can be more extensive and may lead to bleeding, coagulation disorders, or compression of neighbouring organs. Malignant transformation of a haemangioma is extremely rare.
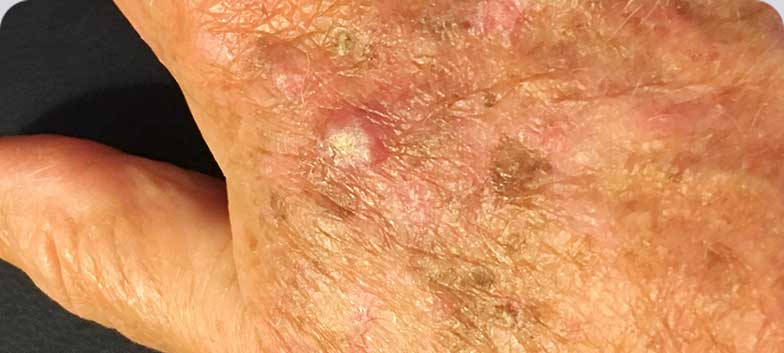
Actinic Keratosis
Actinic keratosis is a red, scaly lesion. It most commonly appears on the face, ears, lips, backs of the hands, forearms, shoulders, décolletage, bald scalp, or other sun-exposed areas. Initially, lesions are small and are often easier to detect by touch, feeling the scaly texture. The presence of actinic keratoses indicates sun damage and these lesions may progress to skin cancer if left untreated.
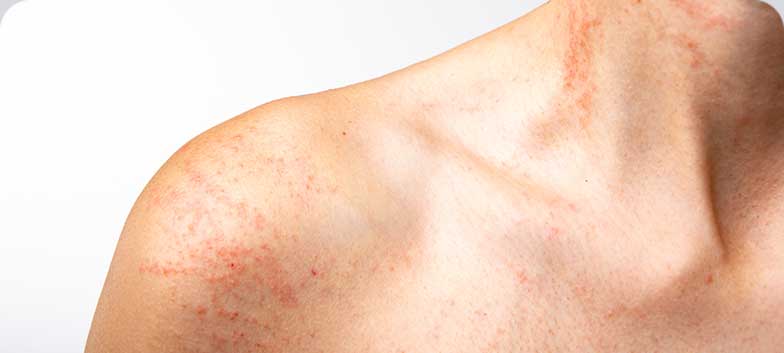
Urticaria
Urticaria presents as red, swollen (edematous) lesions resembling welts, which appear on the skin and cause intense itching. Lesions may be small and isolated or may merge to form large red plaques with varying shapes. Urticaria can appear on any part of the body. Lesions often migrate, with some disappearing while others appear.
Warts
Warts are benign skin growths caused by the Human Papillomavirus (HPV). The infection occurs in the outer layers of the skin or mucosa, triggering abnormal cell growth. While generally not serious, warts can be uncomfortable, particularly on sensitive areas such as the soles of the feet, potentially causing pain and affecting walking.

Vitiligo
Vitiligo is a chronic condition characterised by the loss of skin pigmentation. Lesions occur due to a decrease or absence of melanocytes (the cells responsible for producing melanin, the pigment giving skin its colour). The exact cause is not fully understood, but autoimmune alterations appear to be associated with vitiligo. Emotional stress or trauma may also trigger or worsen the condition.
The most common venereological conditions include:
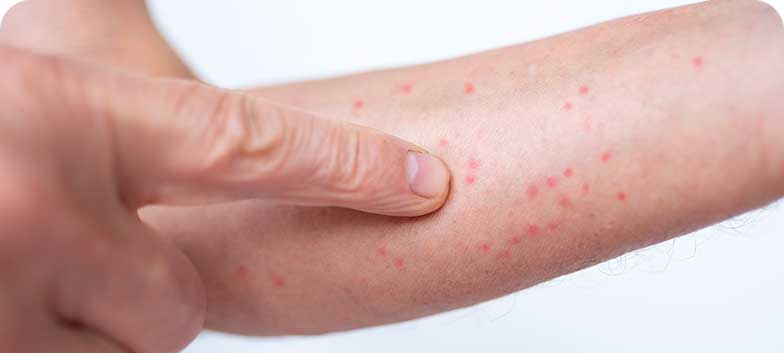
Scabies
Scabies is one of the most common human parasitic infestations, caused by the mite Sarcoptes scabiei var. hominis, which only parasitises humans. In adults, it can be acquired through sexual contact or in family environments. The parasite burrows into the skin, causing an allergic reaction.

Sexually Transmitted Infections (STIs
STIs are transmitted from infected individuals to their sexual partners during vaginal, anal, or oral sex. They are caused by microorganisms, including bacteria, viruses, and parasites.
Anyone can contract an STI if they have sex with an infected person. Transmission is more likely without condom use or with multiple sexual partners. Even those with a single partner may acquire an STI if that partner has other sexual contacts and becomes infected.
Interventions and Treatments
Skin Biopsies
Small portions of skin are removed under local anaesthesia for histopathological diagnosis.
Conventional Dermatologic Surgery
Used to remove skin lesions, sometimes with simple excision and direct suturing, and other times requiring skin grafts (harvesting skin from other areas) or local flaps to cover defects after the removal of large lesions. Dermatologic surgery also includes nail or hair-related procedures and micrographic surgery for large malignant tumours (Mohs surgery).
Cryotherapy
Involves the application of extreme cold (freezing the skin with liquid nitrogen) to destroy benign lesions and, in some cases, malignant lesions.
Curettage
Removal of small superficial lesions (such as molluscum contagiosum or warts) using a spoon-like instrument with sharp edges.
Electrotherapy
Uses electrical current to destroy small skin lesions (e.g., warts) or, in combination with conventional surgery, to coagulate bleeding blood vessels in the operative field.
Phototherapy / Photochemotherapy
Involves exposure of the skin to ultraviolet light, either alone or following topical or systemic photosensitising medications. Commonly used for psoriasis, adult atopic eczema, vitiligo, and cutaneous lymphomas.
Laser Therapy
Ablative lasers destroy damaged tissue (e.g., benign and malignant tumours, warts, condylomas).
Non-ablative lasers are primarily used in cosmetic procedures (e.g., hair removal, removal of brown spots or angiomas).
Dermocosmetic Techniques
Beyond laser and intense pulsed light (IPL), other procedures include chemical peels, dermabrasion, botulinum toxin injections, and dermal fillers (injectable substances such as hyaluronic acid). These are regularly performed by dermatologists to improve the cosmetic appearance of skin conditions or photoageing.
Examinations / Diagnostic Tests:
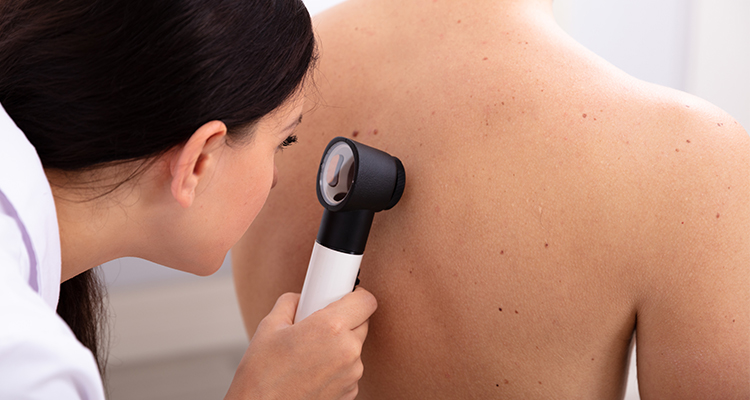
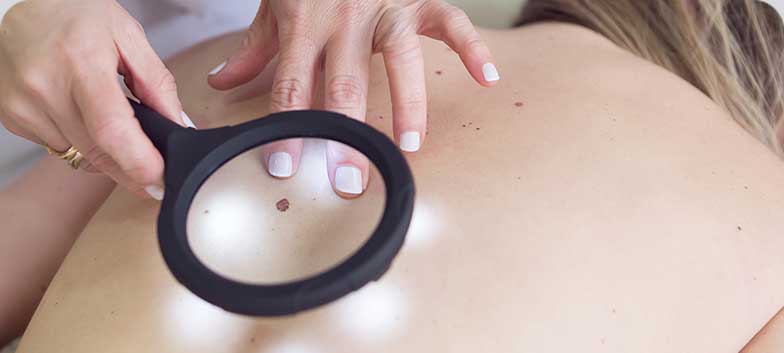
Dermatoscopy
Mainly used to characterise skin lesions. Involves observing the deeper layers of the skin using magnification and specialised lighting, either with a manual or digital dermatoscope. Digital devices allow recording and monitoring of lesion characteristics over time.
Reflectance Confocal Laser Microscopy (RCLM)
Examines the epidermis and papillary dermis with near-histological resolution, allowing visualisation of microanatomical structures and individual cells at high resolution.
Skin Observation
Sometimes performed using magnifying lenses and special lighting.
Patch Testing / Allergy Tests
Used to study contact dermatitis. Adhesive patches containing allergens are applied to the patient’s back for 2 days, after which the skin is examined to determine which allergens cause a reaction.
Photosensitivity Tests
Includes phototesting and photo-patch testing, which expose the skin to various types of light (ultraviolet, visible, or infrared) to assess the immediate and delayed skin response (after 1–2 days).
HPA Dermatology Specialists